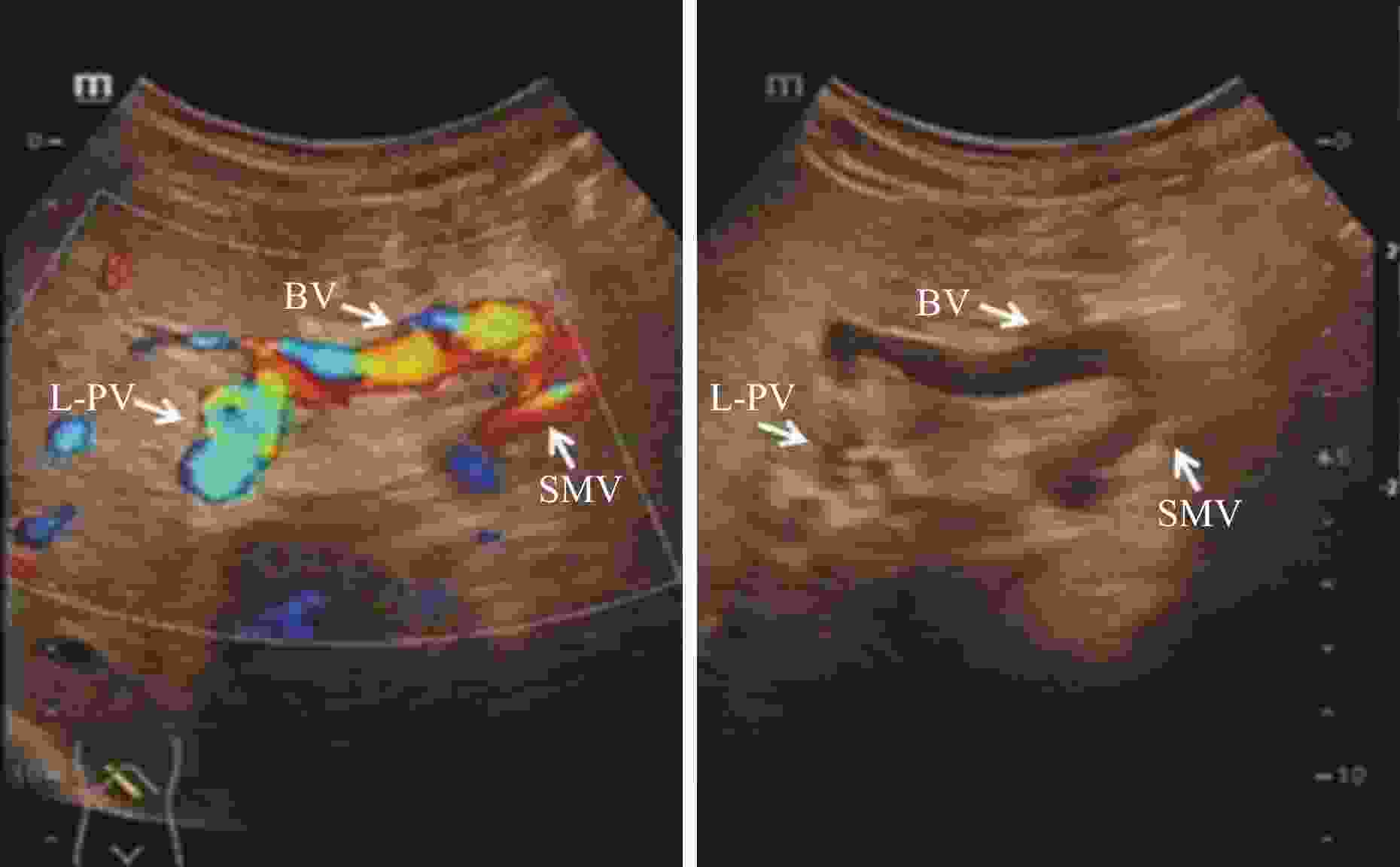
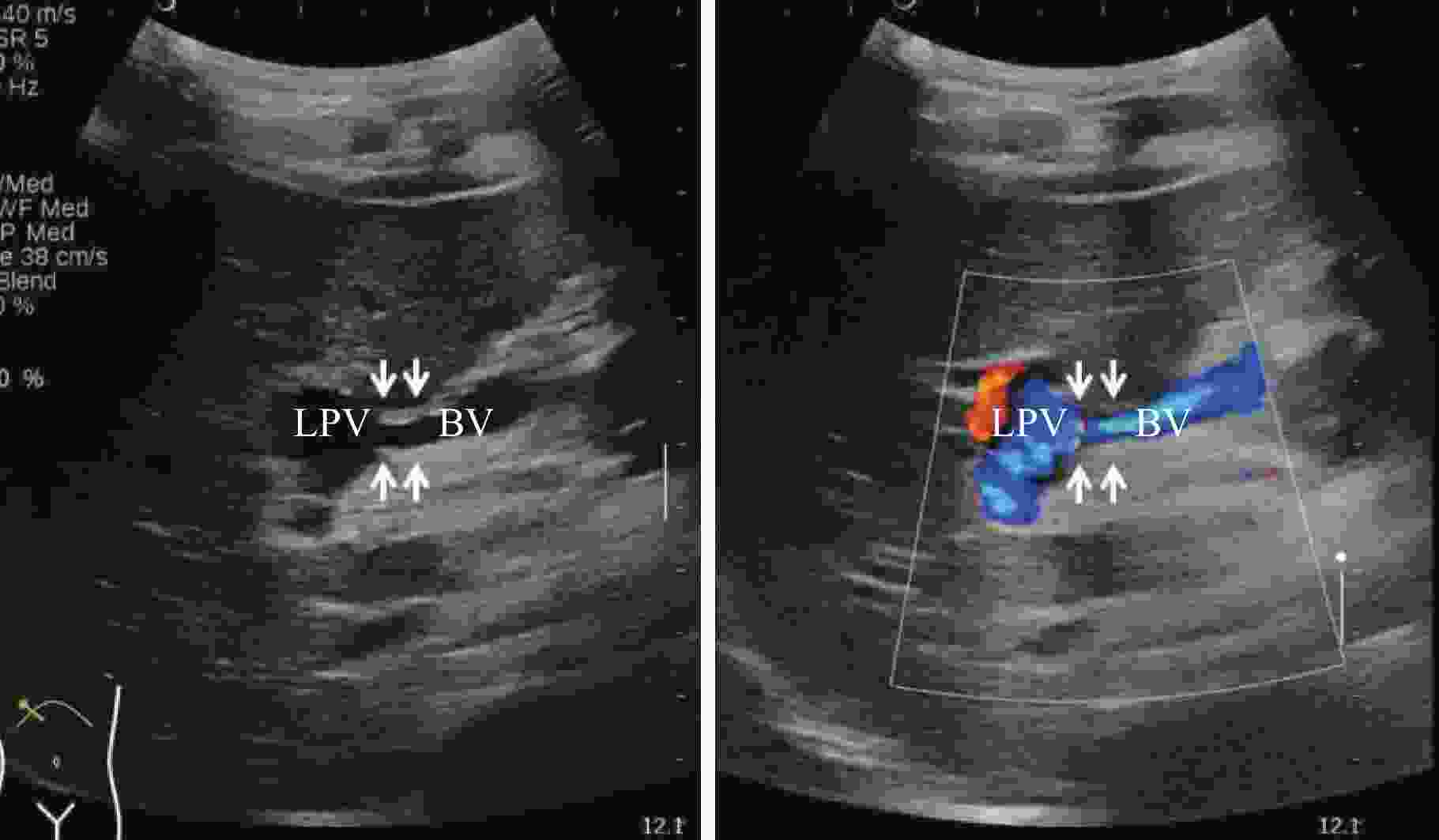
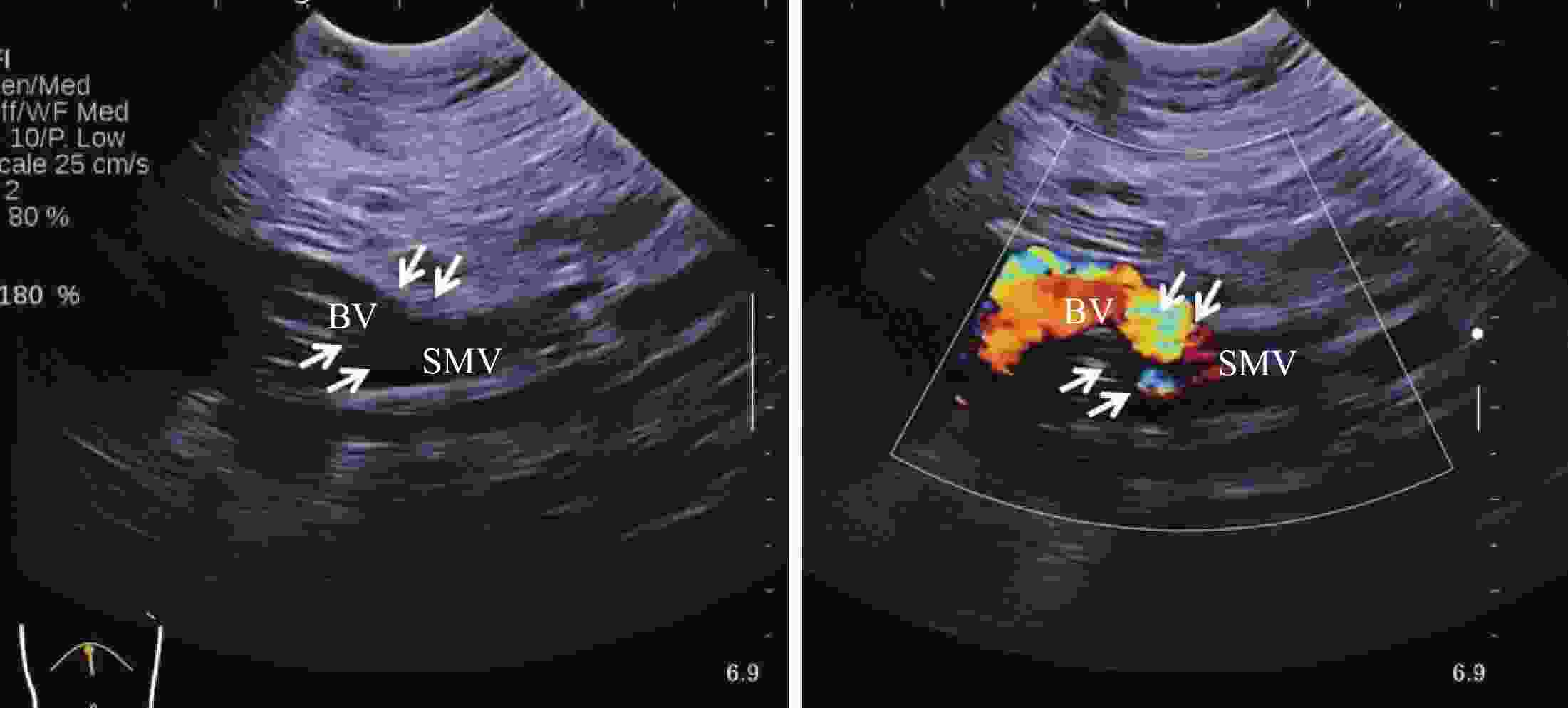
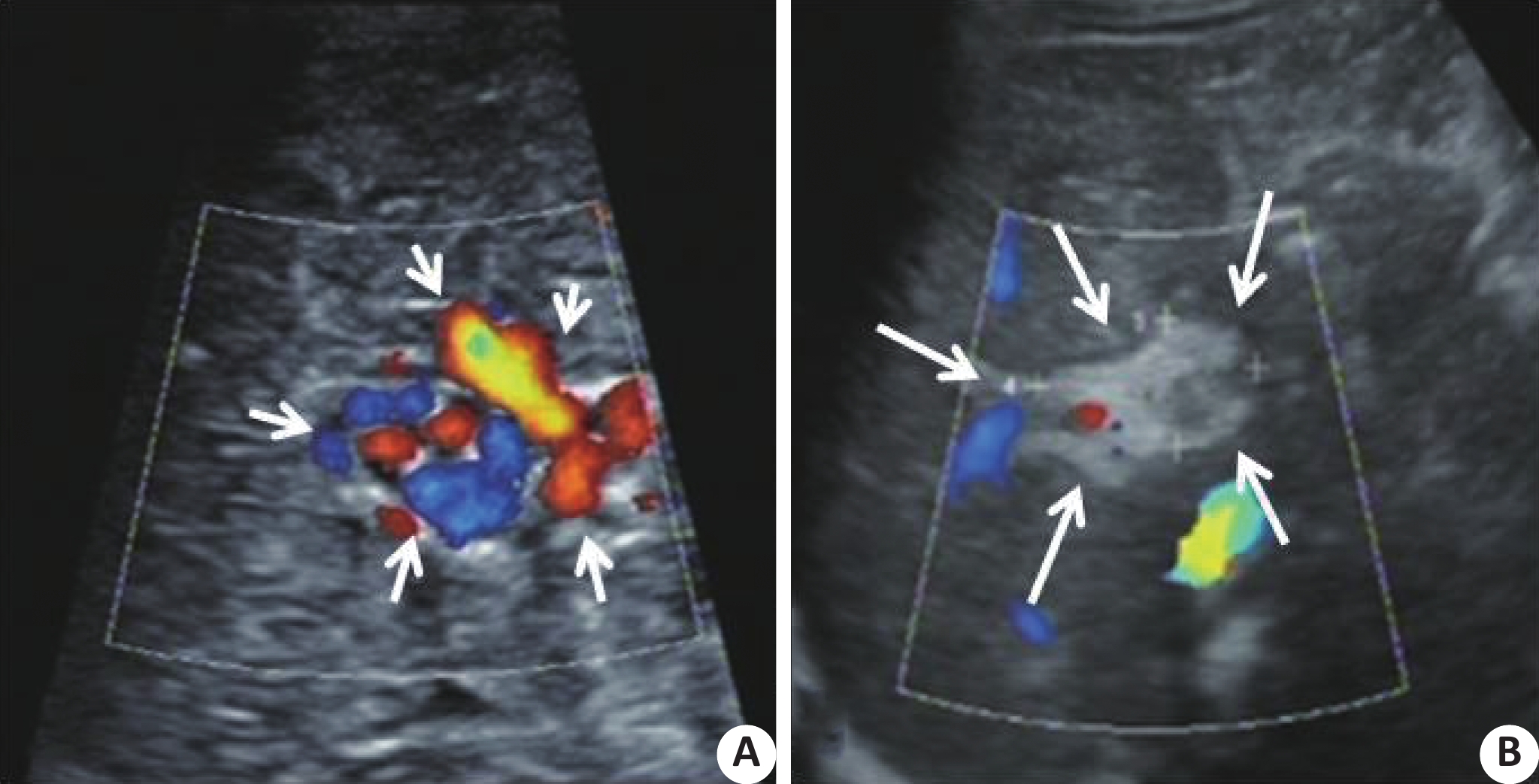
Ultrasound application before and after left portal vein shunt surgery for cavernous portal vein degeneration combined with portal hypertension
-
摘要:
目的探讨超声评估门静脉海绵样变性合并门静脉高压症患儿门静脉左支分流手术(Rex手术)疗效的价值。 方法选取2014年10月~2016年1月在我院因门静脉海绵样变性合并门静脉高压症行Rex手术的患儿10例,手术前、后二维超声分别测量肝脏、脾脏各个径线值并计算其大小变化,测量手术前后门静脉左支、术后桥血管及吻合口内径,多普勒超声评价门静脉左支、桥血管及吻合口的血流通畅情况。 结果10例患儿Rex术后门静脉海绵样变性病变区域血流信号显著减少;术前肝右叶斜径、肝左叶上下径、脾脏面积分别为98.5±3.5 mm、53.3±2.7 mm、42.9±5.9 cm2,其中,术后1周的肝右叶斜径(109.3±1.9 mm)以及术后1年的肝右叶斜径(108.7±1.0 mm)、左叶上下径(64.0±2.5 mm)、脾脏面积(28.5±3.6 cm2)较术前的差异均有统计学意义(P<0.05)。术后门静脉左支、门静脉左支吻合口超声显示清晰,显示率为100%,肠系膜上静脉吻合口显示率为70%。术前门静脉左支内径为2.58±0.34 mm,术后门静脉左支内径为5.33±0.61 mm(术后6月)、6.90±0.95 mm(术后1年),较术前差异均有统计学意义(P<0.05);术后1周、3月、6月、1年的相关血管内径如下:桥血管:5.96±0.80、6.90±0.68、7.41±0.56 mm;门静脉左支吻合口:2.77±0.37、2.71±0.36、3.53±0.32 mm;肠系膜上静脉吻合口:3.26±0.16、3.40±0.17、3.63±0.11 mm。 结论超声可无创、定量评估Rex手术前后肝脏和脾脏大小、门静脉左支,术后桥血管、吻合口内径,评估术后门静脉左支、桥血管及吻合口的血流状态,为手术效果的评估提供可靠指标。 Abstract:ObjectiveTo evaluate the value of ultrasonography in evaluating the efficacy of left portal vein shunt (Rex shunt) in children with cavernous transformation of portal vein combined with portal hypertension. MethodsFrom October 2014 to January 2016, 10 children underwent Rex shunt surgery due to cavernous transformation of portal vein combined with portal hypertension in our hospital were selected. The diameters of the liver and spleen were measured by two-dimensional ultrasound before and after surgery, and the size changes were calculated. The left portal vein, postoperative bypass vein and anastomotic diameter before and after surgery were measured. Doppler ultrasound was used to evaluate the flow patency of the left portal vein, bypass vein and anastomotic stoma. ResultsThe blood flow signal in the area of cavernous transformation of portal vein after Rex shunt surgery was significantly decreased in 10 cases. The oblique diameter of the right lobe of the liver, the upper and lower diameter of the left lobe of the liver, and the area of the spleen were 98.5±3.5 mm, 53.3±2.7 mm, and 42.9±5.9 cm2 before the operation, respectively. The oblique diameter of the right lobe of the liver (109.3±1.9 mm) one week after the operation and the oblique diameter of the right lobe of the liver (108.7±1.0 mm), upper and lower diameter of the left lobe (64.0±2.5 mm), and the area of the spleen (28.5±3.6 cm2) one year after the operation had significant statistical significance compared with that before the operation (P < 0.05). After the operation, the anastomotic stoma of the left portal vein and the left portal vein was clearly displayed by ultrasound, the display rate was 100%, and the display rate of the anastomotic stoma of the superior mesenteric vein was 70%. The diameter of the left portal vein before operation was 2.58±0.34 mm, and the diameter of the left portal vein after operation was 5.33±0.61 mm (6 months after operation) and 6.90±0.95 mm (1 year after operation), both of which were statistically significant (P < 0.05). At 1 week, 3 months, 6 months and 1 year after surgery, the diameter of the relevant vessels was as follows: bypass vein: 5.96±0.80 mm, 6.90±0.68 mm, 7.41±0.56 mm; Anastomosis of the left portal vein: 2.77±0.37 mm, 2.71±0.36 mm, 3.53±0.32 mm; Anastomosis of the superior mesenteric vein: 3.26±0.16 mm、3.40±0.17 mm、3.63±0.11 mm. ConclusionUltrasound can evaluate the size of liver and spleen, left portal vein before and after Rex shunt surgery, postoperative bypass vein and anastomotic diameter, and postoperative blood flow status of the left portal vein, bypass vein and anastomotic stoma, providing reliable indicators for the evaluation of surgical effect. -
表 1 手术前后肝脏、脾脏各项测值(Mean ± SD)
Table 1. Measured values of liver and spleen before and after operation
组别 肝右叶斜径(mm) 肝左叶前后径(mm) 肝左叶上下径(mm) 脾脏厚径(mm) 脾脏最大长径(mm) 脾脏面积(cm2) 术前 98.5±3.5 38.8±1.7 53.3±2.7 44.3±3.7 117.3±6.7 42.94±5.87 术后1周 109.3±1.9* 39.7±1.5 58.2±1.5 42.8±3.6 114.1±6.5 4 155±586.0 术后3月 103.4±2.6 40.6±2.1 57.0±2.3 41.4±3.7 112.4±5.7 3 852±538.5 术后6月 107.0±2.7 40.2±1.7 60.3±2.5 37.6±3.7 102.8±4.7 3 203±455.6 术后1年 108.7±1.0* 43.2±2.0 64.0±2.5* 34.7±2.8 99.7±5.1 2 846±356.3* *P< 0.05 vs术前. 表 2 门静脉左支、桥血管及吻合口的测值(Mean ± SD, mm)
Table 2. Measurement of left branch of portal vein, bridge vessel and anastomosis
组别 门静脉左支 桥血管 门静脉左支吻合口 肠系膜上静脉吻合口 术前 2.58±0.34 — — — 术后1周 3.86±0.33 5.96±0.80 2.77±0.37 3.26±0.16 术后3月 4.59±0.38 6.90±0.68 2.71±0.36 3.40±0.17 术后6月 5.33±0.61* 7.41±0.56 3.53±0.32 3.63±0.11 术后1年 6.90±0.95* 7.50±0.54 3.53±0.28 3.75±0.08 *P< 0.05 vs术前. -
[1] 夏 蓓. 门静脉海绵样变性[J]. 小儿超声诊断学, 2013, 2(1): 478-9. [2] Li ZP, Wang SS, Wang GC, et al. Transjugular intrahepatic portosystemic shunt for the prevention of recurrent esophageal variceal bleeding in patients with cavernous transformation of portal vein[J]. Hepatobiliary Pancreat Dis Int, 2018, 17(6): 517-23. doi: 10.1016/j.hbpd.2018.09.008 [3] Mileti E, Rosenthal P. Management of portal hypertension in children[J]. Curr Gastroenterol Rep, 2011, 13(1): 10-6. doi: 10.1007/s11894-010-0151-y [4] Gugig R, Rosenthal P. Management of portal hypertension in children[J]. World J Gastroenterol, 2012, 18(11): 1176-84. doi: 10.3748/wjg.v18.i11.1176 [5] de Ville GJ, Alberti D, Clapuyt P, et al. Direct bypassing of extrahepatic portal venous obstruction in children: a new technique for combined hepatic portal revascularization and treatment of extrahepatic portal hypertension[J]. J Pediatr Surg, 1998, 33(4): 597-601. doi: 10.1016/S0022-3468(98)90324-4 [6] Lv Y, He C, Guo W, et al. Transjugular intrahepatic portosystemic shunt for extrahepatic portal venous obstruction in children[J]. J Pediatr Gastroenterol Nutr, 2016, 62(2): 233-41. doi: 10.1097/MPG.0000000000000982 [7] 戈小虎, 马志刚. 门静脉海绵样变性的外科治疗策略[J]. 国际外科学杂志, 2012, 45(12): 1015-26. [8] Zhang JS, Li L, Cheng W. A new procedure for the treatment of extrahepatic portal hypertension in children[J]. J Am Coll Surg, 2016, 222(6): e71-6. doi: 10.1016/j.jamcollsurg.2016.03.020 [9] Zhang JS, Liu SL. Gastroportal shunt for potal hypertension in children[J]. J Pediatr Surg, 2012, 47(1): 253-7. doi: 10.1016/j.jpedsurg.2011.09.058 [10] Wei Z, Rui SG, Yuan Z, et al. Partial splenectomy and use of splenic vein as autograft for meso-rex bypass a clinical observational study[J]. Med Sci Monit, 2014, 20(9): 2235-42. [11] Cho YP, Ha TY, Ko GY, et al. Use of meso-Rex shunt with transposition of the coronary vein for the management of extrahepatic portal vein obstruction[J]. Ann Surg Treat Res, 2014, 86(2): 105-8. doi: 10.4174/astr.2014.86.2.105 [12] Bhat R, Lautz TB, Superina RA, et al. Perioperaive strategies and thrombophilia in children with extrahepatic portal vein obstruction undergoing the meso-Rex bypass[J]. J Gastrointest Surg, 2013, 17(5): 949-55. doi: 10.1007/s11605-013-2155-z [13] Lautz TB, Sundaram SS, Whitington PF, et al. Growth impairment in children with extrahepatic portal vein obstruchion is improved by mensenterico-left portal vein bypass[J]. J Pediatr Surg, 2009, 44(11): 2067-70. doi: 10.1016/j.jpedsurg.2009.05.016 [14] Superina R, Bambini DA, Lokar J, et al. Correction of extrahepatic portal vein thrombosis by the mesenteric to left portal vein bypass[J]. Ann Surg, 2006, 243(4): 515-21. doi: 10.1097/01.sla.0000205827.73706.97 [15] Zhang JS, Li L, Cheng W. Optimal procedure of modified Rex shunt for the treatment of extrahepatic portal hypertension in children[J]. J Vasc Surg Venous Lymphat Disord, 2017, 5(6): 805-9. doi: 10.1016/j.jvsv.2017.02.011 [16] Zhao H, Tsauo J, Zhang X, et al. Regarding "the optimal procedure of modified Rex shunt for the treatment of extrahepatic portal hypertension in children"[J]. J Vasc Surg Venous Lymphat Disord, 2018, 6(3): 421-2. doi: 10.1016/j.jvsv.2017.11.008 [17] Bambini DA, Superina R, Almond PS, et al. Experience with the Rex shunt (mensenterico-left portal bypass) in children with extrahepatic portal hypertension[J]. J Pediatr Surg, 2000, 35(1): 13-8. doi: 10.1016/S0022-3468(00)80005-6 [18] Superina R, Shneider B. Emre S, et al Surgical guidelines for the management of extra-hepatic portal vein obstruction[J]. Pediatr Transplant, 2006, 10(8): 908-13. doi: 10.1111/j.1399-3046.2006.00598.x [19] Chiu B, Superina RA. Encephalophalopathy caused by a splenorenal shunt can be reversed by performing a mesenteric-to-left portal vein bypass[J]. J Pediatr Surg, 2006, 41(6): 1177-9. doi: 10.1016/j.jpedsurg.2006.01.075 [20] Macías Rodríguez MA, Rendón Unceta P, Navas RC, et al. Ultrasonography in patients with chronic liver disease: its usefulness in the diagnosis of cirrhosis[J]. Rev Esp Enferm Dig, 2003, 95(4): 258-64. [21] Alexander R. Cortez, Al-Faraaz Kassam, et al The role of surgical shunts in the treatment of pediatric portal hypertension[J]. Surgery, 2019, 166(5): 907-13. doi: 10.1016/j.surg.2019.05.009 [22] Zhang JS, Li L, Hou WY, et al. Spleen-preserving proximal splenic-left intrahepatic portal shunt for the treatment of extrahepatic portal hypertension in children[J]. J Pediatr Surg, 2015, 50(6): 1072-5. doi: 10.1016/j.jpedsurg.2015.02.048 [23] Facciuto ME, Rodriguez-Davalos MI, Singh MK, et al. Recanalized umbilical vein conduit for meso-Rex bypass in ertrahepatic portal vein obstruction[J]. Surgery, 2009, 145(4): 406-10. doi: 10.1016/j.surg.2008.12.004 [24] Chiu B, Pillai SB, Sandler AD, et al. Experience with altermate sources of venous inflow in the meso-Rex bypass operation: the coronary and splenic veins[J]. J Pediatr Surg, 2007, 42(7): 1199-2202. doi: 10.1016/j.jpedsurg.2007.02.033 -






 下载:
下载: